Tamara Rosner, Health, Medicine & Veterinary Science co-editor
Your body plays host to millions of bacteria. In fact, the number of bacterial cells in your gastrointestinal (GI) tract is about equal to the number of cells that make up your body.
While we typically think of bacteria as “bad” or “unhealthy”, the bacteria that make up our gut microbiome are incredibly important in keeping our bodies functioning. They protect us from unwanted pathogens and are important for a healthy immune system. They also impact how our food is broken down and digested. Most important, unbalanced or low-diversity microbiomes are associated with a variety of health concerns, such as diabetes, obesity, colorectal cancer, and irritable bowel syndrome.
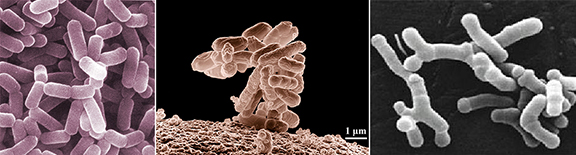
Good gut bacteria: Lactobacillus (Flickr, CC BY-SA 2.0), Escherichia coli (Wikipedia, Public Domain) and Bifidobacteria (Wikimedia, CC BY-SA 3.0)
Recent research has explored the link between gut microbiota and mental health. It demonstrated that the GI bacteria living in mice could greatly impact their brain function and mental well-being. For a variety of tasks, mice with low microbiome diversity displayed greater levels of anxiety and depression than mice with typical microbiomes. For example, anxiety was measured in mice using the forced swim test. Each mouse was placed in water, and those that took longer to begin actively swimming were assumed to be “frozen in place” due to stress. Mice with low diversity in their GI tracts took longer to start swimming – that is, were deemed to be more stressed – than typical mice in the experiment.
Other work shows that administering beneficial probiotics (a mixture of bacteria) to mice with low microbiome diversity can normalize their levels of anxiety and depression, and can even reduce signs of stress in healthy mice.
But what does this research say about how the humanmicrobiome impacts our mental health? This question has captivated many Canadian researchers at the University of British Columbia, McMaster University, and York University. Their research shows associations between gut bacteria and anxiety, depression, alcohol dependence, and susceptibility to post-traumatic stress disorder in humans.
Probiotic use has been linked to lowered stress response in both healthy individuals and those with a clinical diagnosis. But before you go reaching for your yogurt to help reduce your stress, note that these findings are very preliminary. Most of the studies have small sample sizes, and there is little consistency in the makeup, dosage, and time course of the probiotics used. It is even unclear if the probiotics are more effective ingested in a pill or a special mixture of yogurt. Still, this research demonstrates a promising avenue that may help us better understand the complexities of mental health.
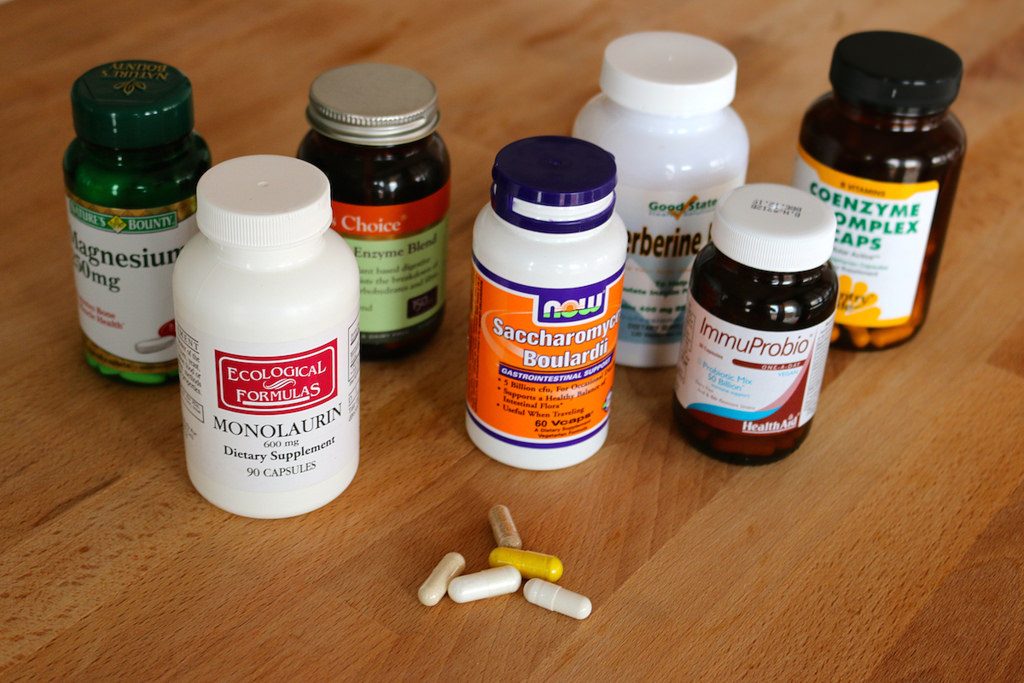
It is unclear if probiotics pills or special yogurt mixes are more effective treatment methods. (Flickr, CC BY 2.0)
These findings also suggest we may one day employ a more…unconventional form of mental health treatment: fecal transplants. In a fecal transplant, fecal bacteria from a healthy donor are inserted into the patient’s gut to overwhelm infectious bacteria and restore a healthy microbiome. The procedure is already being used to treat gut infections caused by antibiotic resistant bacteria.
If an unbalanced microbiome can impact mental health, fecal transplants from a healthy individual may improve mental health symptoms in someone else. The first study to examine this possibility is currently being conducted at the Women’s College Hospital in Toronto, led by Dr. Valerie Taylor. The goal of this work is to see if fecal transplants can improve symptoms of bipolar depression, and the results could lead to new ways of promoting mental health.
Of course, there is still much that is not known regarding the connection between the gut microbiome and mental health and brain function. For one thing, it’s unclear exactly howbacteria in our guts impact our brain. One possible pathway is through the vagus nerve, which connects the brain to many organs, including our guts. The vagus nerve is thought to control hunger, inflammatory responses, and gut movement, but it might also receive signals from the gut microbiome that affect brain function. In addition, it is not clear how different strains and species of bacteria might impact mental health.
Since this is a new area of research, there are many questions to be asked. While we still don’t know exactly how the microbiome communicates with the brain, there does seem to be a strong connection between what is in our gut and how we think, feel, and behave. It seems that a “gut feeling” could one day take on a whole new meaning.
~30~




